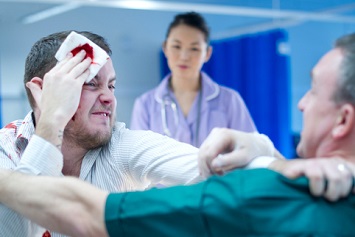
As have other organizations that advocate for healthcare workers, the Joint Commission is strongly urging healthcare organizations to take a comprehensive look at the occurrence of violence against their employees and take steps toward implementing protections that “look beyond solutions that only increase scrutiny.”
To that end, the Commission has published a Sentinel Event Alert, Physical and Verbal Violence Against Health Care Workers, “to help your organization recognize and acknowledge workplace violence directed against health care workers from patients and visitors, better prepare staff to handle violence, and more effectively address the aftermath.”
The alert summarizes issues that make healthcare workers among the most victimized classes of employees, the particular challenges of tracking assaults on workers (mainly because of “gross underreporting” by the workers themselves), and seven specific actions the Commission recommends that employers undertake or enhance.
The Joint Commission is an independent, not-for-profit organization that accredits and certifies nearly 21,000 healthcare organizations and programs in the United States.
Defining Violence
One of the critical issues in workplace violence is defining precisely what constitutes an episode of violence that employees should report and that employers should formally record and subject to a “comprehensive systematic analysis.” The Commission’s policy states that rape, assault (leading to death, permanent harm, or severe temporary harm), or homicide of a patient, staff member, licensed independent practitioner, visitor, or vendor while on-site at an organization is a sentinel event that warrants analysis. But it is critical that the definition of workplace violence does not stop there.
“It is up to every organization to specifically define acceptable and unacceptable behavior and the severity of harm that will trigger an investigation,” says the Commission. “Recognizing verbal assault as a form of workplace violence cannot be overlooked, since verbal assault is a risk factor for battery. According to the ‘broken windows’ principle, apathy toward assaults such as verbal abuse creates an environment conducive to more serious, physical crimes.”
Recommended Actions
The Commission suggests that healthcare employers take the following actions:
- Clearly define workplace violence, and put systems into place across the organization that enable staff to report instances of workplace violence, including verbal abuse. For example, create simple, trusted, and secure reporting systems that result in transparent outcomes and are fully supported by leadership, management, and labor unions. Also, protect patient and worker confidentiality in all reporting by presenting only aggregate data or removing personal identifiers.
- Recognizing that data come from several sources, capture, track, and trend all reports of workplace violence, including verbal abuse and attempted assaults when no harm occurred. Gather this information from all hospital databases, including those used for OSHA, insurance, security, human resources, complaints, employee surveys, legal or risk management purposes, and from change-of-shift reports or huddles.
- Provide appropriate follow-up and support to victims, witnesses, and others affected by workplace violence, including psychological counseling and trauma-informed care if necessary.
- Review each case of workplace violence to determine contributing factors. Analyze data related to workplace violence and worksite conditions to determine priority situations for intervention. Review workers’ compensation, insurance records, OSHA logs, and other data relating to workplace violence, and analyze where, when, why, and how violence has occurred and to whom.
- Develop quality improvement initiatives to reduce incidents of workplace violence. Such initiatives typically include changes to the physical environment and changes to work practices and administrative procedures.
- Train all staff, including security, in de-escalation, self-defense, and response to emergency codes. Regarding de-escalation and self-defense, experts suggest that hospitals prohibit firearms from campus, except for firearms used by law enforcement officers. The Centers for Medicare and Medicaid Services (CMS) does not permit the use of weapons by any hospital staff as a means of subduing a patient.
- Evaluate workplace violence reduction initiatives. Specific actions include surveying workers to determine the effectiveness of initiatives and partnering with local law enforcement or having a consultant review the worksite.
The Commission’s alert contains additional information for each of the above suggestions.